A report by the World Health Organisation in 2018 found that 630 million children under the age of five are exposed to air pollution worldwide

Asthma is a common lung condition that causes occasional breathing difficulties - and is often diagnosed during childhood (Credit: Wikimedia)
Air pollution is causing more children across the world to be diagnosed with respiratory problems like asthma, according to new analysis.
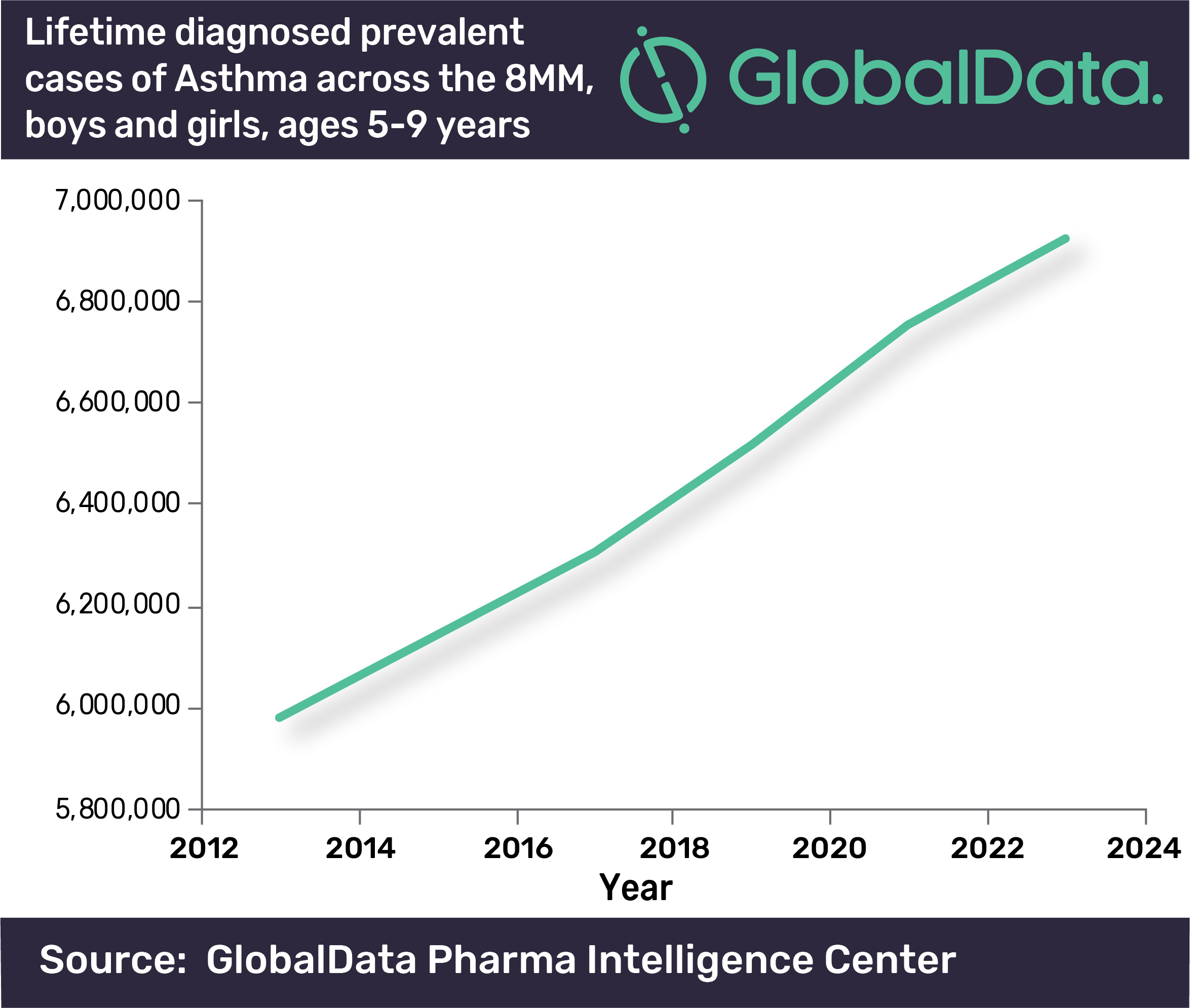
Data analytics company GlobalData estimates the number of children aged between five and nine living with asthma in parts of Europe, Asia and the US will reach about seven million in 2023.
In 2013, this was closer to six million, but analysts predict this has increased by 1.6% each year – and will continue to do so with many people being exposed to toxic air.
The number of children dying due to lower respiratory tract infections (RTIs) – conditions affecting the throat, airways, lungs or sinuses – is also increasing, which has led to GlobalData calling air pollution a public health threat.
The company’s associate epidemiologist Katie Wrenn said: “Air pollution is largely the result of population growth, increased energy consumption and industrialisation in cities.
“While the highest levels of air pollution are currently seen in low and middle-income countries, low-level air pollution in high-income countries is also considered a public health concern.
“It is vital that all countries have policies in place to control levels of air pollution and in turn reduce the number of children suffering from respiratory problems.”
Why is air pollution considered a public health threat for children?
In October 2018, a report by the World Health Organisation (WHO) estimated that 93% of boys and girls under the age of 15 worldwide are breathing toxic air.
This equates to roughly 1.8 billion children having either short or long-term exposure to air that’s so polluted, it can directly contribute to asthma and RTIs, as well as decreasing lung function.
This number includes 630 million children under the age of five.
WHO also stated that air pollution is one of the leading threats to child health and accounts for about one in 10 deaths in children under five.
Lower RTIs – particularly serious forms of respiratory infection – were estimated by WHO to have caused 600,000 child deaths in 2016.
In 2016, WHO announced it would be leading the BreatheLife campaign, which lays out policy measures for governments across the world to adopt in order to hit WHO air quality targets by 2030.
The United Nations Environment Programme (UNEP) and the UN’s Climate and Clean Air Coalition (CCAC) are also leading the campaign alongside WHO.
It aims to increase monitoring of cities and governments, and educate people about the threat air pollution poses towards their health.
The countries involved in the campaign include the UK, Mexico, India and Canada – as each have air quality goals based on their individual needs.
Can technology help reduce air pollution exposure for children with asthma?
Asthma is a condition in which a person’s airways narrow and swell, producing extra mucus that can make breathing difficult and trigger coughing, wheezing and shortness of breath.
Treatment usually involves daily medication that reduces inflammation, as well as “rescue medicine” in the form of an inhaler or injections that, in the case of a more serious episode, relax the muscles and open them up.
But scientists have begun to develop various new technologies that can help prevent asthma attacks.
The University of North Carolina’s School of Medicine has teamed up with software developer SAS to develop personalised technology that can predict when a patient could experience an asthma attack.
Patients that have taken part in the research project are supplied with devices that are designed to be worn all the time and are equipped with physiological, biochemical and environmental sensors.
The scientists found that personalised monitoring of the pollutant gas ozone could help prevent asthma attacks.
Speaking at the IoT Solutions World Congress in Barcelona in October, Dr Michelle Hernandez, an associate professor specialising in allergies and immunology at the University of Carolina, said higher levels of ozone led to significant drops in lung function over time.
“It emphasised that medication isn’t enough – we need to try to reduce the exposure, which is where mobile technology can help,” she said.
“The ultimate goal for me is if we can tell if a person is going to be sick and needs help, then we can try to prevent those emergency care visits and have the best life possible.”
The University of Texas’ Dell Medical School, meanwhile, has worked with the fellow Austin-based People’s Community Clinic to build a system that integrates non-medical information like weather, air pollution and pollen count into a patient’s electronic medical record.
It helps clinicians understand how issues such as exposure to smoke and pollen, housing conditions and transportation accessibility – which research suggests influence more than 80% of a person’s overall wellbeing – could lead to an asthma attack.
The school’s dean dean Dr S Clairborne “Clay” Johnston told NS Healthcare: “Our goal is to get the data to predict who’s most at risk and then try to prevent it by providing the best treatment within a few hours of it happening.”